Great advances have been made in the field of breast surgery; however, for some cases (male and female) the most appropriate treatment remains a mastectomy. Such a decision would be made where the cancer is close to, or includes the nipple, or where a large tumour is present in a person with a small breast.
Post-operative choices and techniques
All units carrying out breast surgery should have a breast care specialist nurse attached. This specialist nurse is able to advise on all aspects of breast care from diagnosis, through surgery and treat¬ment, to advice on post-operative treatment and care, including the use of bras and prostheses.
Breast prosthesis
Following a mastectomy your relative will be offered a prosthesis, an artificial breast worn inside the bra. Prostheses are made of soft silicone in a range of sizes, shapes and colours, to achieve as nat¬ural a look as possible. Immediately after the operation your relative may be given a soft, light fabric prosthesis to wear until her chest wall has healed completely. Women who wish to augment a small breast reconstruction can use a partial prosthesis. The structure allows the prosthesis to fit neatly and safely into a bra, with a nipple outline to give a well-balanced appearance.
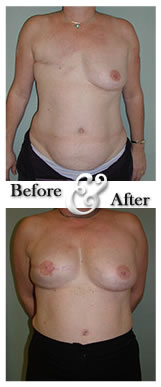 Methods and timing
Methods and timing
Reconstruction of a breast(s) may be performed after a mastecto¬my or lumpectomy to restore the breast to a size and shape that is similar to the original. Several methods are used according to which technique (or combination of techniques) best suits the area on which the surgeon must work, and taking into account the wishes of the patient. Much help and advice will be offered by the cancer team before and after the operation.
The timing of the reconstruction also depends on several factors; for example, some surgeons prefer to do all the surgery at one time, whereas others recommend a time gap to allow the operation site to recover; radiotherapy and chemotherapy usually mean a delay of several months. Your relative’s views will always be sought and at this emotional time she may need extra support and the chance to talk over the options. The waiting lists for breast recon¬struction surgery are quite long in some areas.
The idea of a breast reconstruction is attractive for many women, particularly if they are very concerned by the thought of a trau¬matic change in body shape or by the bother of dealing with a separate prosthesis (artificial replacement). The psychological and practical advantages of a permanent reconstruction outweigh the disadvantages because dressing is easier and body image more acceptable. However, it is important to understand that the new breast will not be identical to the one removed during surgery -the new tissue will be less sensitive and the reconstructed shape of the flesh and nipple will look different. Once your relative is fully dressed the appearance is very agreeable, with little outward sign that the two breasts differ.
Occasionally cosmetic surgery work is performed on the healthy breast to make it easier for the surgeon to match the new recon¬struction; for example, the existing breast may be reduced in size or lifted. Additional surgery for cosmetic effect would only be done after discussion about the advantages and disadvantages for your relative.
Reconstruction techniques
There are two main types of reconstruction performed in the UK using implanted, artificial material or a tissue flap using transplanted tissue taken from elsewhere in the body.
An artificial implant uses either saline (salt) fluid or silicone gel inserted into the body within a textured, silicone casing. The saline fluid is a natural substance, so it is less likely to cause problems if it seeps out, but a saline-type implant feels less realistic than a silicone model. Encapsulated silicone gel implants have been used for many years and there is little risk associated with this type of procedure. The main problems highlighted in the media have been linked to use of silicone injections where a compound was inject¬ed directly into breast tissue. Reports of leakage and infection caused women to be fearful of the technique, with claims of auto¬immune disorders developing. The use of silicone injections is now banned in the UK and the USA and monitoring of all silicone implants is undertaken regularly by the Department of Health. Fol¬lowing a review in 1998 the report found that ‘there is no good evidence of an abnormal immune response … and there is no rea¬son to stop using silicone implants’ (CancerBACUP).
After-care
Immediately after the surgery the area will be taken care of by nurs¬ing staff, who will advise on personal hygiene. For example, showers are better than baths and careful drying of the area is important. Many doctors advise gently massaging the area daily with oils or creams to keep the skin soft and elastic, and to help reduce the amount of fibrous tissue that can form around the capsule.
A support bra worn during the day and at night time is suggested by some surgeons to help reduce the dragging, whereas another school of thought recommends wearing a normal bra or none at all to encourage the new breast to develop its own natural shape. Your relative must be guided by her own surgeon. Full movement is usually recovered after about six weeks. A physiotherapist will teach suitable arm exercises to aid mobility. It is important to con¬tinue to observe the reconstructed breast regularly for signs of change and the breast care nurse will tell your relative what to look out for.
